
Antibiotics are a type of antimicrobial medication used to treat infections caused by bacteria. In the 1930s, a sulfonamide was the first commercially available product to treat infections caused by Gram-positive bacteria. In the mid-1940s, penicillin was introduced on a large scale, marking the beginning of the antibiotic era. Following their discovery and development into products for human and animal health, multiple antibiotics have been used to treat bacterial infections by either preventing the formation of the cell wall, which effectively kills the bacteria (bactericidal effect), or stopping their replication (bacteriostatic effect).
This article aims to highlight how to successfully navigate the challenges of antibiotic-free and reduced antibiotic use in the poultry industry, as well as provide a closer look at the history and development of these dynamic production programs.
Antibiotic Resistance and foodborne illness
Antibiotic resistance is an ancient, naturally occurring phenomenon that evolved long before antibiotics were available to treat human or animal diseases. It occurs when a bacterial organism develops the ability to resist the effects of one or multiple antibiotics to which they were once sensitive. As a result, diseases caused by antibiotic resistant bacteria are difficult to treat, leading to persistent infection, severe clinical signs, higher treatment costs and increased mortality.
Antibiotic resistance is an increasingly serious global threat to both public and animal health, and therefore, it is widely recognized that steps must be taken to reduce the use of antibiotics while allowing their use in a judicious manner and preserving their continuous efficacy. Antibiotic resistance can be described as a type of microbial warfare, by which some microorganisms gain a selective advantage by producing their own antibiotics that either inhibit or eliminate other competing bacteria. Although antibiotic resistance occurs naturally, numerous studies have highlighted that lack of research, difficulties in developing new antibiotics, inadequate disease prevention and misuse in humans and animals are accelerating the process.
The development and increasing frequency of antibiotic resistance has led to concerns about foodborne diseases caused by enteric pathogens. Enteric bacteria such as Salmonella and Campylobacter, commonly found in poultry, can spread to people through contaminated food products. Campylobacter is a leading foodborne pathogen carried in the intestinal tract of a wide range of domestic and farm animals, including poultry, wild animals and birds. A growing number of Campylobacter resistant strains have been reported in the USA, Canada and Europe. Other enteric bacteria contain enzymes that allow them to become resistant to various penicillins and cephalosporins. Non-typhoidal Salmonella species can be resistant against ceftriaxone, ciprofloxacin and several other antibiotics.
 The most severe and hard-to-treat infections by enteric pathogens are caused by carbapenem-resistant bacteria, which have become resistant to nearly all antibiotics available today. In 2013, the US Department of Health and Human Services, Centers for Disease Control and Prevention (CDC), estimated that microorganisms from food and animals caused 1 in 5 resistant infections in people.
The most severe and hard-to-treat infections by enteric pathogens are caused by carbapenem-resistant bacteria, which have become resistant to nearly all antibiotics available today. In 2013, the US Department of Health and Human Services, Centers for Disease Control and Prevention (CDC), estimated that microorganisms from food and animals caused 1 in 5 resistant infections in people.
To combat the threat of infectious disease spreading between animals and people, the World Health Organization (WHO) recommended a holistic and multifactorial approach called “One Health”. One Health consists of a collaborative, multisectoral and transdisciplinary methodology, implemented on a local, national, and global scale to achieve the best outcomes for people, animals, plants and the environment. Figure 1 shows the connection between human, animal and environmental health of this strategy, which is widely supported and considered necessary for controlling the spread of antibiotic resistance and ensuring the future of safe and sustainable animal food production.
Antimicrobial Resistance and consumer perception
Antimicrobial is a term used to describe medications that work against various microorganisms such as bacteria, viruses, fungi and parasites. Antimicrobial resistance is a broader term used to describe resistance to medications against bacteria and other microorganisms such as fungi, parasites and viruses. Therefore, antibiotic resistance is a component of antimicrobial resistance, regularly used in scientific and popular literature to refer to the emergent and growing threat of diverse resistant microorganisms besides bacteria.
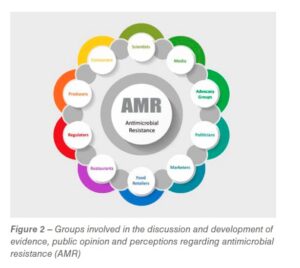
There is an increasing discussion about the potential dangers of animal food products contaminated with “superbugs” that could cause severe illnesses. Although there has been limited evidence, recent documented episodes of foodborne disease attributed to poultry products have increased unfavorable perceptions and decreased customer confidence. Consequently, all these issues have captured the attention of politicians, marketers, retailers and restaurants that are well attuned to customer demands and business opportunities. Regulatory agencies have set new restrictions and requirements, which continue to be updated and modified to ensure food safety. Figure 2 shows the main groups involved in the discussion and evolution of public opinion and perception.
 There is rising interest in alternative products, which has created a thriving new industry and the availability of numerous products with various purported beneficial attributes that can be used in animals of all ages. Research and development of alternative products (immune modulators, phytochemicals, probiotics, prebiotics, normal gut flora, yeast extracts, etc.) to reduce the need for and use of antibiotics in food animals have demonstrated some benefits. Although results vary, and further research is needed to maximize their benefits under different field conditions, alternative products are being used alone, or most commonly in combinations, by producers worldwide as part of comprehensive health management programs.
There is rising interest in alternative products, which has created a thriving new industry and the availability of numerous products with various purported beneficial attributes that can be used in animals of all ages. Research and development of alternative products (immune modulators, phytochemicals, probiotics, prebiotics, normal gut flora, yeast extracts, etc.) to reduce the need for and use of antibiotics in food animals have demonstrated some benefits. Although results vary, and further research is needed to maximize their benefits under different field conditions, alternative products are being used alone, or most commonly in combinations, by producers worldwide as part of comprehensive health management programs.
Animal agriculture in general, and specifically poultry producers, have responded to public health concerns and consumer demands by implementing prudent guidelines for the judicious use of antibiotics and production strategies that eliminate or minimize the need for them. Whether or not these changes in animal food production will reduce antimicrobial resistance risk and impact on the human population remains to be demonstrated. However, a new era characterized by significant antibiotic usage reduction and/or antibiotic-free poultry production has arrived. Today there is an even stronger commitment by producers and poultry professionals to protect public health and promote transparency and communication with customers.
Ethical poultry stewardship
Veterinary and health organizations around the world agree on the importance of the judicious use of antibiotics. These organizations continue to advocate effective use through carefully planned and executed practices in areas such as vaccination, health monitoring, diagnostics, biosecurity, husbandry and management programs.
Poultry veterinarians work with flocks of domestic poultry rather than individual animals. Therefore, poultry veterinarians must:
- Conduct medically appropriate and timely visits to the facility where poultry flocks are housed.
- Examine representative patients/birds and review medical records and laboratory or diagnostic procedure records.
- Consult with those individuals providing care to the birds regarding ongoing health management programs.
For each specific antibiotic or antimicrobial used in food-producing animals, regulatory requirements establish a particular time of “no antibiotic use”, also known as the “withdrawal period” before harvest. This period is the time required for the bird to eliminate these products from their systems, so no residues are present when animals are processed for human consumption. Therefore, veterinarians assist producers by ensuring that antimicrobials are administered in compliance with withdrawal times established for specific products. Additional oversight (verification of compliance) is conducted by regulatory agencies involved in the monitoring, detecting and controlling residues in poultry products. Interestingly, many retailers and consumers in the United States are not aware that due to regulatory requirements, all chicken meat sold contains no antibiotics or residues, and that all flocks are raised under health programs designed by licensed poultry veterinarians.
In Europe and other parts of the world, there is a similar legislation requiring that all antibiotics are prescribed by a veterinarian who must follow specific guidelines. They may only prescribe antibiotics for poultry under their care, and there are specific guidelines for when the poultry are placed in the care of a named veterinarian. Additionally, industry bodies such as the Responsible Use of Medicines in Agriculture Alliance (RUMA) in the United Kingdom have been in action for many years. RUMA is an associate member of the European Platform for Responsible Use of Medicines in Animals (EPRUMA). European veterinary organizations like the British Veterinary Poultry Association (BVPA) also have specific guidelines for antibiotic use that are regularly updated, with the last update published in 2018.
Despite all of the on-going industry and veterinary efforts to prevent poultry diseases, some flocks become sick, and antibiotic treatment is a necessary and justifiable option for the poultry veterinarian. A growing trend in the food supply chain (i.e. food retailers and restaurants) is the requirement for poultry meat or eggs produced with no antibiotics ever (NAE), and in general, these products command a premium price. As a result, when a flock becomes sick and must be treated with antibiotics for health and welfare reasons, its products cannot be labeled as NAE and enter that market. Consequently, this creates an economic dilemma for the producers when a flock becomes sick and must be treated with antibiotics since its meat or eggs have to be diverted to other acceptable market sectors. These are typically sold at a lower price – despite complying with required withdrawal periods and freedom of residues before entering the food chain.
Veterinarians take an oath guiding and affirming their use of scientific knowledge and skills for the benefit of society by protecting animal health and welfare, the prevention and relief of animal suffering, the conservation of animal resources, the promotion of public health and the advancement of medical knowledge. Therefore, veterinarians must be able to prescribe proper treatment plans for animal health and animal welfare, including the use of an antibiotic when this option is justified, to conform with their professional commitment and ethical obligation. Antimicrobial stewardship is a shared responsibility for veterinarians, regulatory agencies, and poultry production managers. Commitment to the use of antimicrobials in a judicious manner and continuous collaboration among all stakeholders is essential to ensure poultry welfare and the industry’s future.
Challenges and opportunities of antibiotic-free and reduced antibiotic use production
The shift to antibiotic-free/reduce antibiotic US production has come with some challenges. Several reports suggest that raising chickens without antibiotics could reduce performance compared with traditional programs (i.e. unrestricted access to judicious use of all approved medications). This is possibly due to higher mortality because of neonatal infections and/or a higher incidence of intestinal health problems such as coccidiosis and necrotic enteritis. Also, concerns about negative impacts on animal welfare have been raised. Discernibly, there has been a learning curve since the start of antibiotic-free/reduced antibiotic use production, and broiler operations worldwide continue to identify key factors, upgrade their practices, develop new disease prevention strategies and make gradual improvements.
More recent studies and field experiences have shown that it is possible to achieve similar performance and cost-efficiency as traditional systems in the absence of antibiotics. During the last few years there has been an abundance of scientific and industry publications on strategies to make antibiotic-free/reduced antibiotic use production successful. Achieving this goal depends on a comprehensive review and improvements in the following areas:
- Management practices (breeders, hatchery, and broilers).
Chick quality. - House environmental controls.
- Litter management and treatments.
- Water quality, diet composition and feeding practices.
- Gastrointestinal development and health (including gut microbiota).
- Biosecurity, downtime between flocks, cleaning and disinfection practices.
- Control of coccidiosis and necrotic enteritis.
- Prevention of immunosuppressive conditions.
- Use of alternative products (feed additives to promote gut health).
- Monitoring of flock behavior, health and performance (transition times).
- Pre-harvest food safety.
The broiler industry continues to thrive and, as the world population grows, the demand for safe, affordable and nutritious animal protein continues to rise, particularly in developing economies around the world. Poultry products continue the trend to become the protein of choice on a global basis. Consequently, poultry professionals and production managers will likely be confronted with additional customer and regulatory requirements. The industry must continue to evolve through innovation, communication, transparency and technology.
Conclusion
Navigating the course of an ever-evolving industry can seem like a daunting task. However, by focusing on attention to detail, a firm commitment to bird welfare and the responsibility of ethical poultry stewardship, it is possible to successfully face the opportunities and challenges presented by antibiotic-free/reduced antibiotic use poultry production.
Here you can find the full article: http://ap.aviagen.com/assets/Tech_Center/Broiler_Breeder_Tech_Articles/English/Focus-ABF-History-2021-EN.pdf








